Endometriosis & Adenomyosis
Painful periods and painful sex are definitely not normal!
Tele-Health
Endometriosis consultations are now available with our specialised Women's Sexual Health GPs
Endometriosis (pronounced “End-oh-meet-ree-oh-sis”) and 'un-affectionately' known as "Endo", is relatively common, with an estimated one in nine Australian women suffering from the condition.
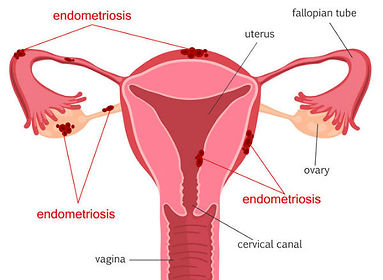
It occurs when tissue similar to the lining of the womb (uterus) starts to grow in other places, such as the lining of the pelvis or sticking to organs in the pelvis such as the ovary or fallopian tubes.
Endometriosis can affect women of any age, but is most common in women in their 30s and 40s. Adenomyosis (often referred to as Endo's ugly big sister) is typically found in women between the ages of 35 and 50, but also affects younger women.
They are both long-term conditions, which are not life-threatening but can have a significant impact on the quality of life of those afflicted, due to the debilitating pain and other symptoms that they can cause.
2600 women submitted our Endometriosis Symptom Questionnaire, and the results are truly devastating
The endometriosis questionnaire is designed to have the participant answer many of the questions that a trained specialised sexual health GP would ask when exploring a possible endometriosis or adenomyosis prognosis.
Looking at the aggregated data and scanning the individual submissions (without actually speaking to all of them), it would appear that a significantly large percentage of the 2600 were ‘likely’ suffering with endometriosis, while a good portion presented characteristics more in line with adenomyosis.
Overwhelmingly, what came through loud and clear from the submissions is the heartbreaking reality that they feel helpless, hopeless and are not receiving the answers and the professional care they need. Many women reported feeling that they were being ignored and discarded by their healthcare providers.
On behalf of our profession and as women’s health GPs, we find this absolutely unacceptable, and why we have introduced our 'Is it Endometriosis? via Telehealth' service.
Symptoms of Endometriosis
The symptoms of endometriosis can vary. Some women are badly affected, while others might not have any noticeable symptoms. Some women have endometriosis and don’t know about it.
The main symptoms of endometriosis are:
-
pain in your lower tummy, back or pelvic pain– usually worse during your period
-
period pain which is so severe that stops you doing your normal activities
-
pain during or after sex
-
pain when peeing or pooing during your period
-
feeling sick, constipation, diarrhoea, or blood in your pee during your period
-
difficulty getting pregnant
You may also have heavy periods; you might use lots of pads or tampons, or you may bleed through to your clothes.
There is a variation of endometriosis called adenomyosis which is where the lining of the uterus is mixed in with the muscles of the uterus. Adenomyosis can also cause heavy painful periods.
For some women, endometriosis can have a big impact on their life and may sometimes lead to low mood or even depression. This is because it can cause long term pain and be debilitating. There is often a delay in the diagnosis being made.
Diagnosing Endometriosis
It can be difficult to diagnose endometriosis because the symptoms can vary considerably, and many other conditions can cause similar symptoms. That is why making a diagnosis can be tricky and may be delayed.
Though many GPs can miss or mis-diagnose endometriosis and adenomyosis, all of our doctors at Clinic 66 are specially trained and have a special interest in women's sexual and reproductive health. What this means for you is that our GPs are knowledgeable, experienced and well prepared to do an initial assessment and can organise any necessary investigations.
After taking your history and potentially doing a physical examination, your GP may recommend that you try “the pill” or other hormonal treatments, or suggest further investigation such as imaging with ultrasound.
The best way of diagnosing endometriosis is to have a laparoscopy., where a surgeon or gynaecologist passes a thin tube through a small cut in your tummy so they can see any patches of endometriosis tissue. This is the only way to be certain you have endometriosis, and needs to be done in a hospital under a general anaesthetic.
Helping us to Help You
A great place to start is to download the Qendo symptom tracker app. This will be helpful to your GP and/or gynaecologist when an assessment is being undertaken as you can share your information with anyone you choose.
The app is designed to allow you to track the myriad of symptoms that come with endometriosis, adenomyosis, PCOS, infertility and pelvic pain, as well as any other health conditions you may have. Symptoms you can track span both physical and emotional health. Yes, you can track pain, bleeding, bowel and bladder function, headaches, bloating or acne, to name a few; but you can also track stress, energy levels, mental clarity, mood, depression and anxiety, and so much more.

Alternatively, if you prefer the 'old school' way of pen & paper, you can download our printable pain diary.
Dr Emma Boulton debunks some of the most common myths we hear about endometriosis at Clinic 66 and Clinic 66 Online. Our Specialised GPs are extremely concerned about some of the sexual and reproductive health misinformation that is being spread on the socials, and the internet in general. Check your sources before you act on any advice, and if you're not sure, why not make an appointment with one of our telehealth GPs... or just send us a question via the contact form at the bottom of the page!
Although endometriosis is currently not ‘curable’, once a diagnosis is made, treatments are available.
What treatments are available for endometriosis?
There’s currently no cure for endometriosis, but there are treatments that can help ease the symptoms which include:
-
Help with simple management of pain, such as warm packs, gentle exercise
-
Pain relievers – such as ibuprofen, paracetamol and mefenamic acid
-
Hormone medicines and contraceptives – including the combined pill, progestogen tablets such as dienogest, the contraceptive patch or hormonal IUD, and other hormonal medicines
-
Surgery to cut away patches of endometriosis tissue and any scar tissue
-
An operation to remove part or all of the organs affected by endometriosis – such as surgery to remove the womb (hysterectomy). This is usually the last resort.
Your doctor will discuss the options with you. Sometimes they may suggest not starting treatment immediately to see if your symptoms improve on their own. Usually, there is a stepwise approach to treatment to see what works best for you.
What are the risks of having endometriosis?
The biggest problem is that endometriosis can affect your quality of life, primarily due to the pain, and cause you to have days off study or work. It can also affect your sex life if it is painful to have sex.
Sometimes the areas of endometriosis bleed and cause scarring internally. This may require surgery to remove or divide the damaged tissue.
Endometriosis may cause scarring in the fallopian tubes and stop them from transporting an egg during the menstrual cycle.
This may impact on fertility and cause a delay in falling pregnant naturally or an ectopic pregnancy.
Surgery may help fix the scar tissue and help you conceive naturally, but IVF may also be an option if you have been trying for a while.
Do you suspect you may have Endometriosis? Take the Questionnaire...
This questionnaire includes some of the important questions that your GP will ask you whilst investigating your symptoms.
This is by no means a complete diagnostic tool, but simply a 'starting point' to help identify the next steps in your prognosis.
Is it Endometriosis? via Telehealth
We are now offering initial investigative consultations via tele-health online video or telephone appointments with our experienced and understanding sexual health GPs
Telehealth consultations are just like in-clinic consultations, but you will meet with the doctor online via your phone, computer or tablet (no need to come to the clinic for your initial assessment).
You will meet with one of our experienced, knowledgeable and understanding women's sexual health GPs to review your symptoms, conduct an initial assessment and discuss an investigation pathway.
We recommend that you first complete our questionnaire and include your contact details at the end, then download the Qendo App or our printable pain diary (depending on what works best for you) and keep it for at least a week (preferably more) before your appointment.
At Clinic 66, we offer a comprehensive range of services designed to cater to your unique needs such as STD/STI testing, womens health, mens health, sexual health and much more.
Your 30 minute consultation will cost $A$150 and
Medicare will rebate $75.25 = $74.75